Albumin
Primary plasma protein synthesized by the liver. Maintains oncotic pressure and transports small molecules. Low levels suggest liver disease or malnutrition.
Albumin Biomarker Test
Albumin testing provides a window into recovery, resilience, and whole-body health. It helps detect undernutrition, liver strain, protein loss, or dehydration, while also guiding smarter choices in diet, hydration, alcohol use, and training recovery.

Albumin
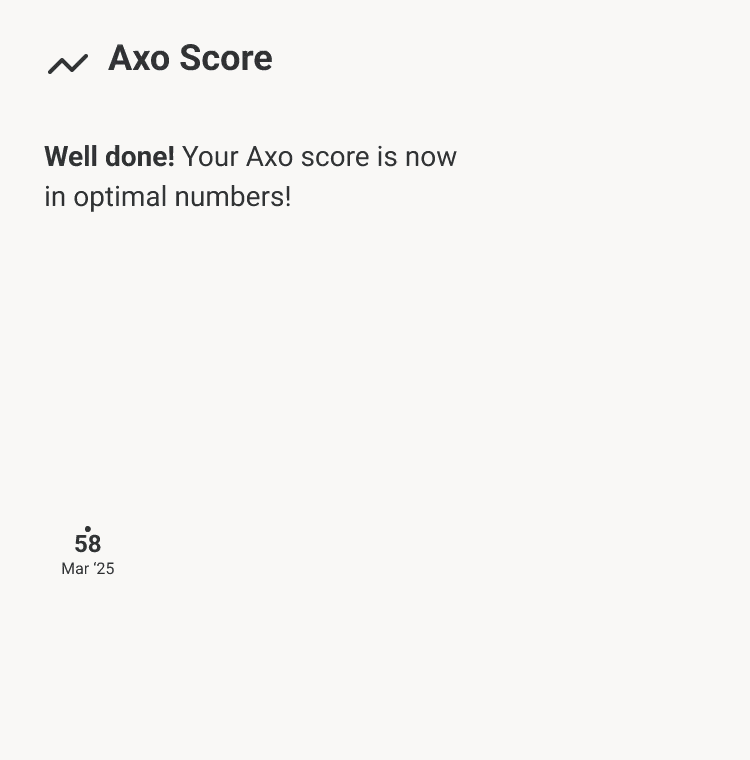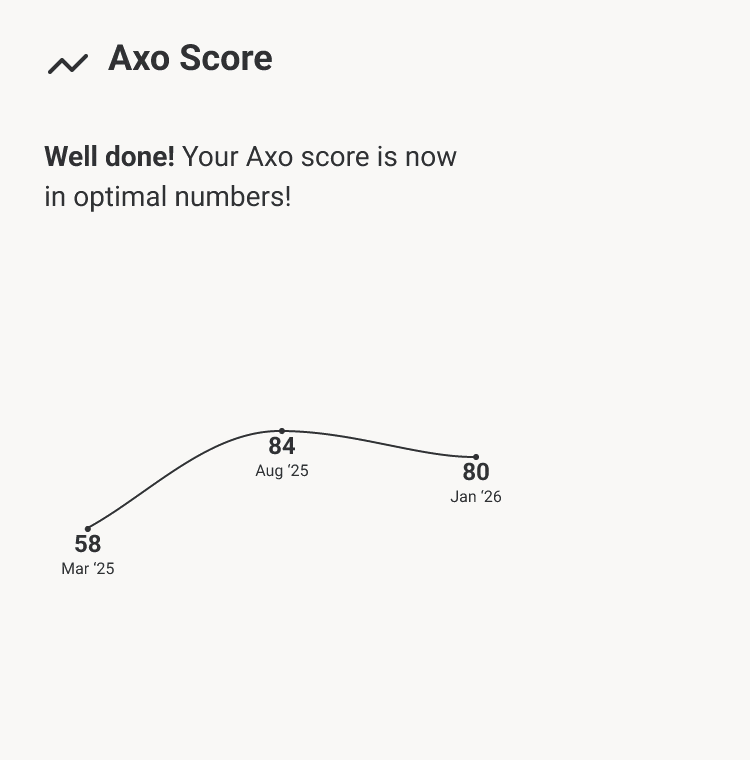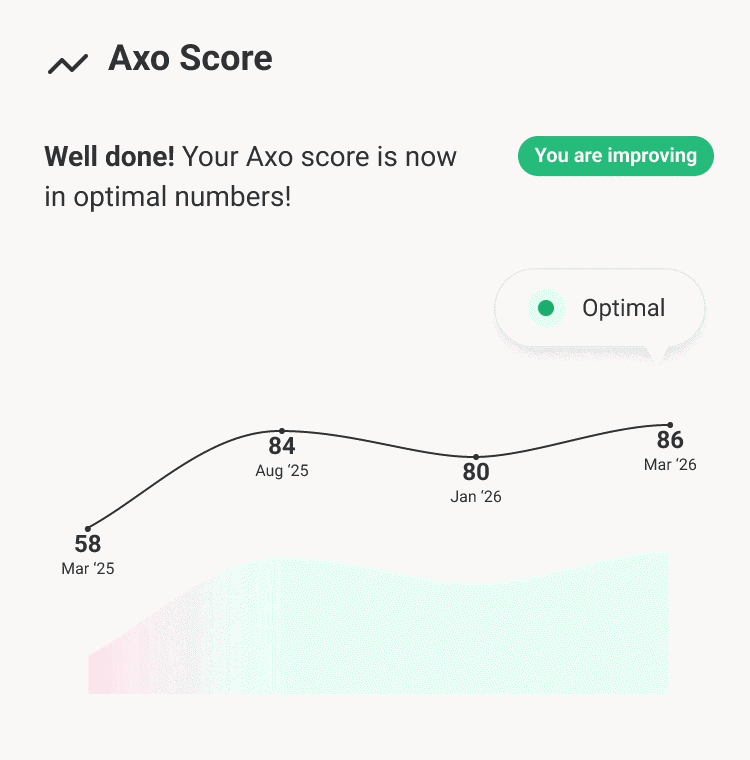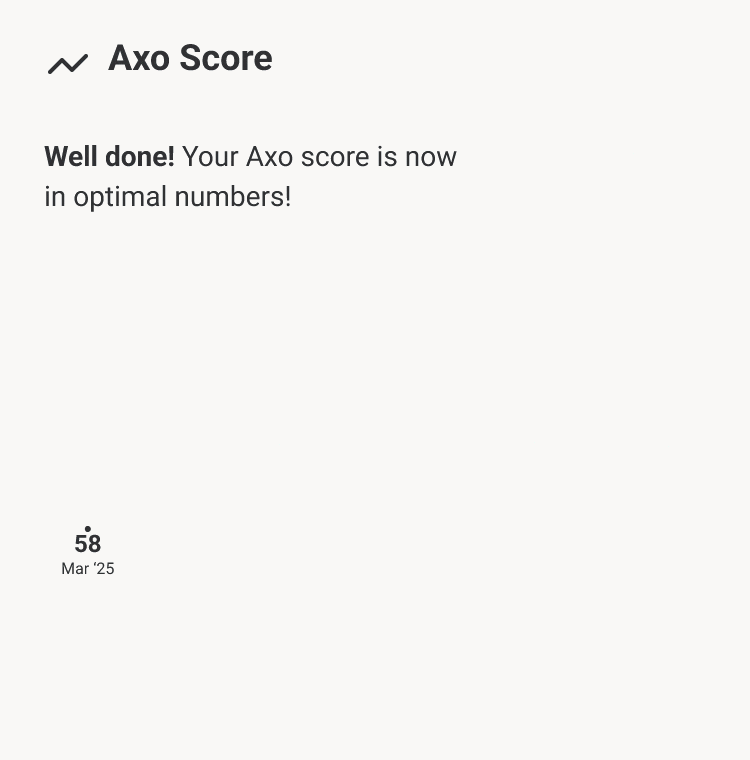
A cycle built for lifelong progress
Each pass deepens the picture, tracks your trajectory, and makes the next recommendation smarter than the last.
If you are in Netherlands, please check the extra step regarding a kit you will receive before going to the lab.
Choose from +450 certified partner labs across Europe. Our first comprehensive draw captures +100 essential biomarkers, everything from cardiovascular markers and metabolic panels to hormone profiles and immune function. You show up. We handle the rest.
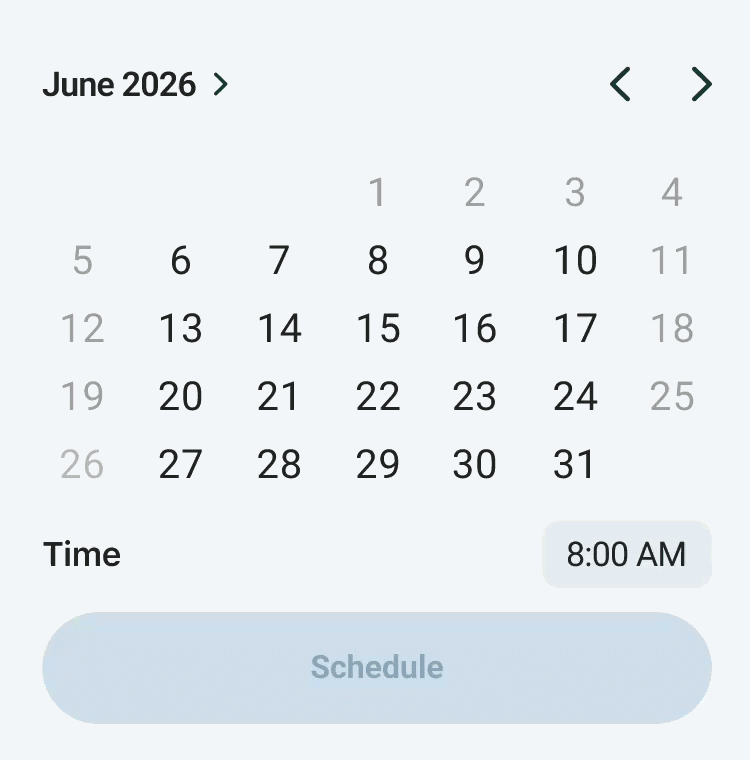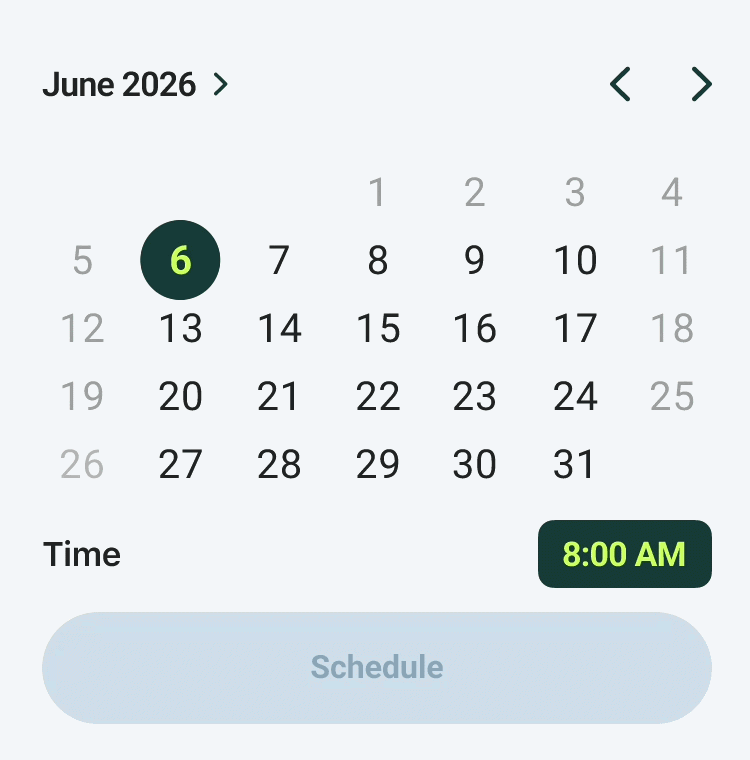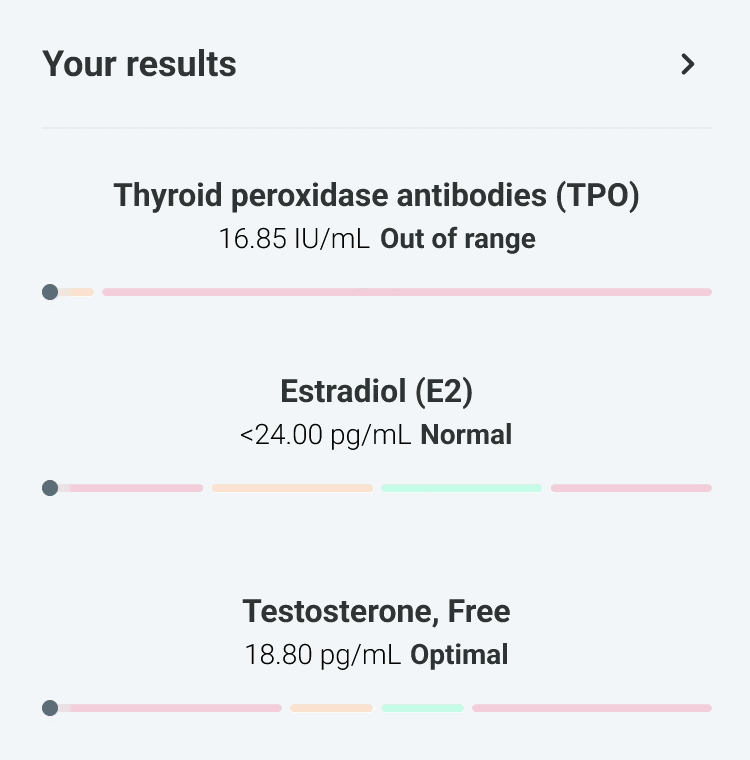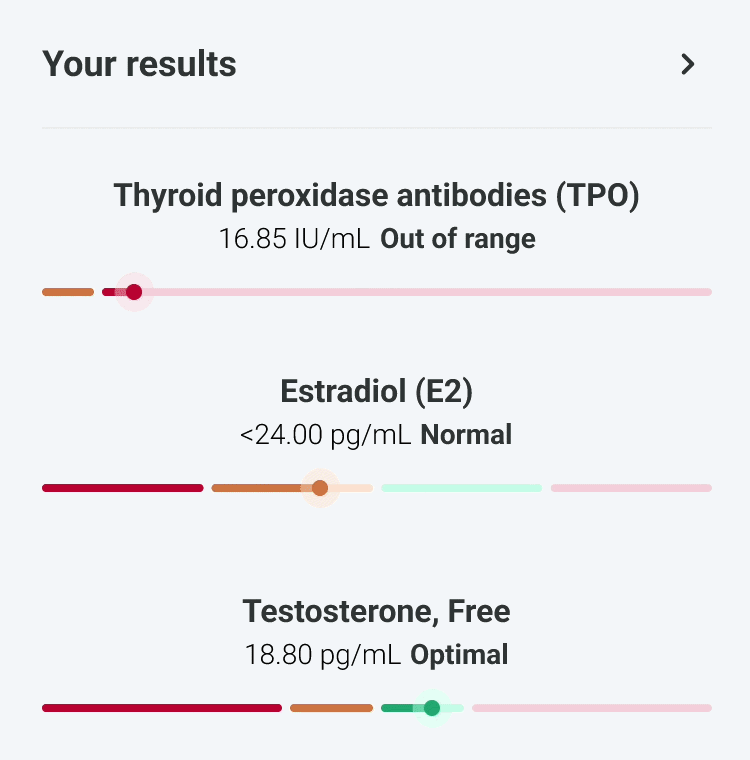
Our experts - not just algorithms - perform a whole-body analysis across cardiovascular, hormonal, metabolic, and immune systems. You receive an Axo Health Score, a Biological Age calculation, and a full breakdown of every marker: what it means, why it matters, and where you stand relative to true optimal ranges - not just lab reference ranges.
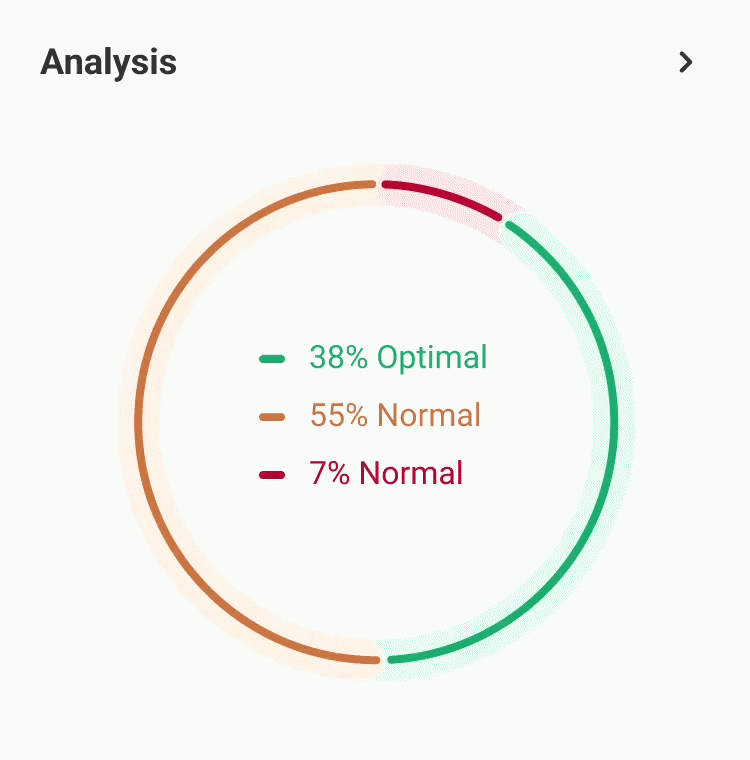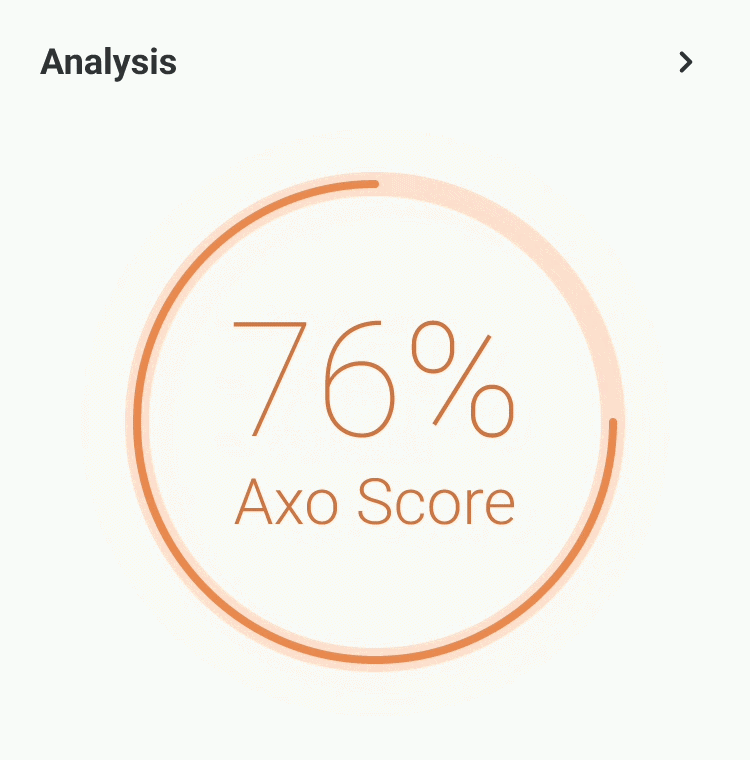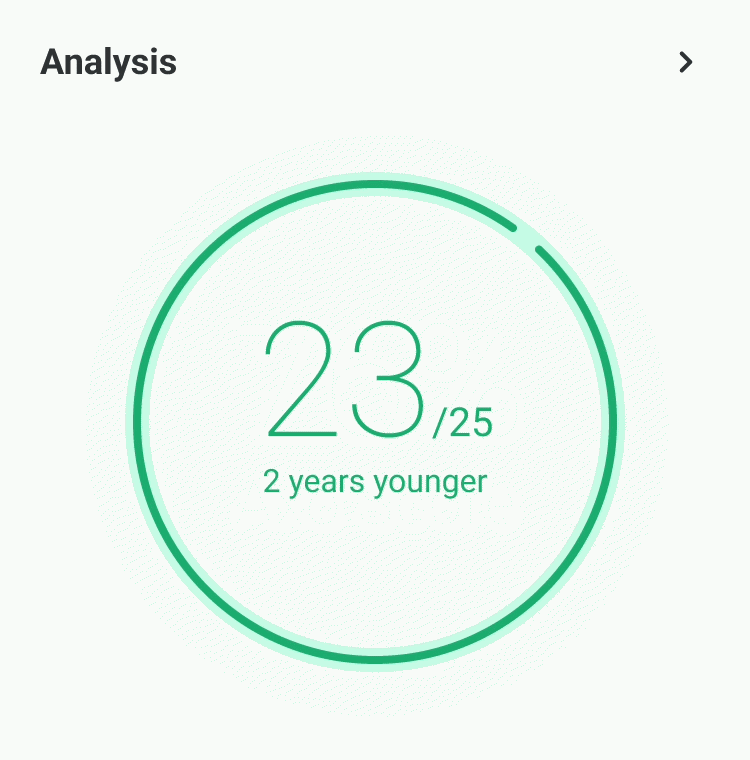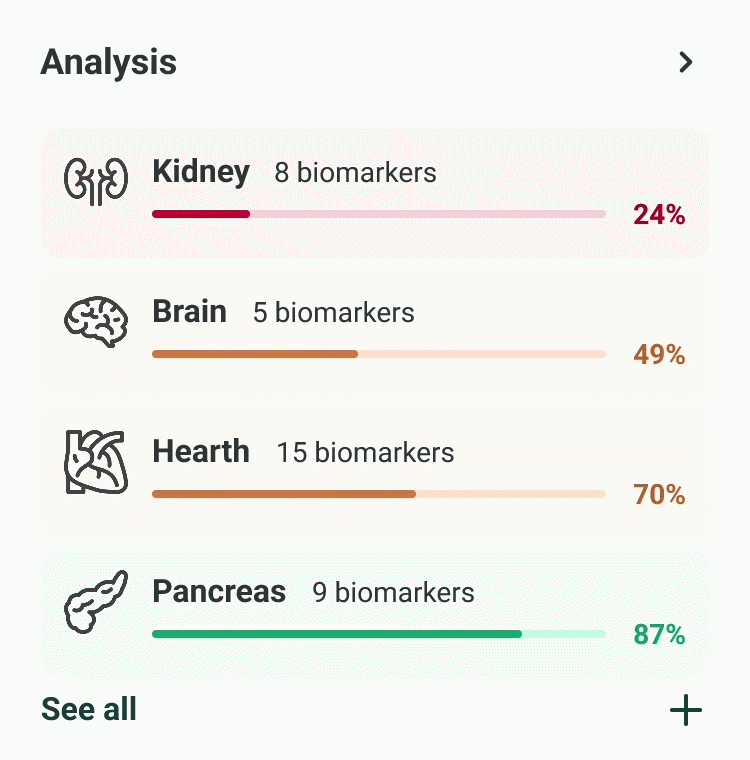
Your personalised health blueprint, built by Dr. Niko Mihic and Dr. Andy Walshe's sports science methodology. Not generic advice - specific, ranked, actionable interventions in nutrition, sleep, supplementation, exercise, and stress. Each recommendation is tied directly to your markers and calibrated to your lifestyle.
At the 6-month mark, a follow-up panel of targeted biomarkers confirms whether your interventions are working. Watch your score improve. See your biological age trend downward. Then the cycle begins again - deeper, sharper, and compounding with every pass.